Ebsteins Anomaly
Download this information sheet as a PDF
The aim of this information sheet is to explain what Ebstein’s Anomaly is, what effect it will have on a child and how it can be treated.
Animation of Ebsteins Anomaly
Animation of normal heart
What is Ebstein’s Anomaly?
Ebstein was a doctor who first named this condition. Anomaly means something which is not usual.
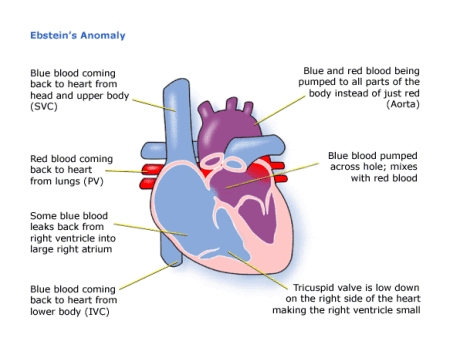
The main features of Ebstein’s Anomaly are:
- The tricuspid valve is abnormal and, instead of being between the right atrium and ventricle, it is low down in the right ventricle.
- The right atrium is large and the right ventricle small. This means that less blue blood is pumped into the lungs.
- There is often a hole between the atria – called the atrial septal defect – which means blue blood may travel through this hole from the right atrium to the left.
- This blue blood is then pumped into the left ventricle, into the aorta and round the body.
How your child may be affected
Ebstein’s Anomaly can range from very mild, with little symptoms, to very severe. How your child is affected will depend on how much blood is able to get to the lungs.
In the milder forms there may be no symptoms at all apart from a heart murmur. Some babies may have a bluish tint (cyanosis). In more severe cases, however, where there is very little blood getting to the lungs, your baby will be very ill at birth and need medical attention straight away.
Diagnosis
Ebstein’s Anomaly can sometimes be picked up before birth on a scan. After birth, if very little blood is getting to the lungs, your child will become very ill as soon as the foetal circulation system (ductus arteriosus) starts closing down. They will start to show signs of heart failure, be sweaty, tired, and look blue (cyanosis).
If your baby has a milder form of the condition, there may not be any symptoms for some years, other than a heart murmur. A heart murmur may be heard as extra blood leaks back through the abnormal tricuspid valve.
When a heart murmur is heard the tests used can be:
- pulse, blood pressure, temperature, and number of breaths a baby takes a minute
- listening with a stethoscope for changes in the heart sounds
- an oxygen saturation monitor to see how much oxygen is getting into the blood
- a chest x-ray to see the size and position of the heart
- an ECG (electrocardiogram) to check the electrical activity
- an ultrasound scan (echocardiogram) to see how the blood moves through the heart
- checks for chemical balance in blood and urine
- a catheter or Magnetic Resonance Imaging test may be needed
In older children, a fast heart rate (tachycardia), shortness of breath and chest pain may be the first symptoms to show.
Treatment
The treatment for Ebstein’s Anomaly will depend on how severe the condition is. Your child’s cardiologist will discuss the treatment options appropriate for your child.
If your child has mild symptoms, he or she will need to be monitored by a paediatric cardiologist, and may never need treatment.
Surgery
If your child has poor oxygen levels, meaning that there is not enough blood getting to the lungs, they will need open heart surgery. This means that their heart will need to be stopped and opened in order to repair it. A machine will have to take over the job that the heart normally does – the heart bypass machine.
The main aim of the surgery will be to get a good supply of blue blood to the lungs to collect oxygen. If the condition is not very severe, then the surgery will:
- repair the atrial septal defect (ASD)
- repair the tricuspid valve, and
- the right atrium will be reduced in size.
Tricuspid valve replacement
Sometimes the tricuspid valve is very deformed, and may need to be replaced by a mechanical (artificial valve). Artificial valves do not grow with the child, so further valve surgery may be needed.
Children with artificial valves will also need to take anticoagulants for the rest of their lives, which can have a number of implications for their health and lifestyle (see the Warfarin Information sheet).
Fontan procedure
In some children with Ebstein’s Anomaly, the right ventricle may be too small to function properly. In this case, the right atrium may be connected directly to the pulmonary artery (Fontan procedure). This means that the blue blood is pushed directly into the pulmonary artery without having to pass through the tricuspid valve and the right ventricle.
BT Shunt and Fontan procedure
If your child has a very severe form of Ebstein’s Anomaly, it may be necessary to have a BT shunt (connection) to increase the amount of blood getting to the lungs shortly after the birth. This is done by connecting a tube from an artery in the arm to the pulmonary arteries. This operation may be carried out through the side of the chest, while the heart is beating, or through the front using a heart lung bypass machine (open heart surgery).
Further surgery (the Fontan procedure), can then be carried out two or three years later. In these cases children may take some time to recover after surgery. The main reason for this is that the pressures in the circulation are changed, and the heart and lungs have to adapt.
How it affects your child
Most children will be much better after treatment. Children who have had surgery to correct the condition are normally completely well shortly after the operation. Most parents are amazed at how quickly their child recovers from surgery and starts to gain weight. There will be a scar down
the middle of the chest, and there may be small scars where drain tubes were used.
These fade very rapidly in most children, but they will not go altogether. Smaller scars on the hands and neck usually fade away to nothing.
Some of these problems can occur after surgery or later in life:
- It is common for the valves to leak a little, but if this becomes severe, they may need further repair or even replacement with an artificial valve. If the valve is replaced, this will need to be monitored to make sure the replacement is working effectively, and an artificial valve may need to be replaced as the child grows. Children with artificial valves will need to take anticoagulants for the rest of their lives, which can have a number of implications for their health and lifestyle (see the Warfarin Information sheet).
- Your child may develop a very fast heart beat (tachycardia) later. This may need to be treated with medicines – anti-arrhythmic drugs.
Evidence and sources of information for this CHF information sheet can be obtained at:
(1) National Institute for Health & Care Excellence. Evidence Search on Ebstein’s Anomaly. London: NICE; 2017. Available at:
www.evidence.nhs.uk/search?q=Ebstein+anomaly
(2) Great Ormond Street Hospital. Factsheet on Ebstein’s Anomaly. London: GOSH; 2017. Available at:
About this document:
Published: June 2013
Reviewed: May 2022
To inform CHF of a comment or suggestion, please contact us via info@chfed.org.uk or Tel: 0300 561 0065.