Dilated Cardiomyopathy
Download this information sheet as a PDF
The aim of this information sheet is to explain what Dilated Cardiomyopathy is, what effect it will have on a child and how it can be treated
What is Dilated Cardiomyopathy?
Dilated cardiomyopathy is a disease of the heart muscle. Dilated means enlarged, cardio concerns the heart and a myopathy is a muscular disease. Dilated cardiomyopathy means that the left ventricle becomes stretched and ‘floppy’. DCM weakens the heart muscle so that it works less efficiently and cannot pump enough blood to the lungs and around the body. This can lead to breathlessness and fluid to build up within the body.
Normal Heart
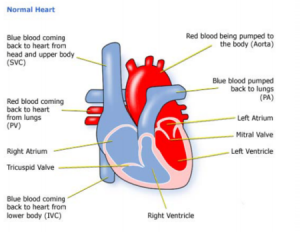
Dilated Cardiomyopathy

What Causes Dilated Cardiomyopathy?
It is not always certain what causes DCM and it can develop at any age. Sometimes dilated cardiomyopathy can be inherited; sometimes it can develop from viral infections, certain medicines, or from autoimmune diseases for example.
How it can affect your child:
- Shortness of breath/tiredness: because the heart is weak, muscles may not receive enough blood to allow your child to run around without quickly becoming exhausted.
- Swelling (oedema): You may notice fluid building up around the ankles/abdomen or other body parts.
- Changes in the heart muscle may interfere with the electrical activity that regulates the heartbeat. Your child may feel that his/her heart is beating too quickly (tachycardia) or too slowly (bradycardia).
- Blood flows more slowly through the heart and this can allow blood clots to form that could cause damage to the lungs, brain or other organs. Your child may need to be treated with anticoagulant medication (Warfarin for example) to prevent such clots from forming.
Diagnosis
DCM is often discovered because a child becomes tired easily, breathless, and perhaps has some swelling caused by fluids building up. There may also be a fast or slow heart beat and the doctor may hear an abnormal heart sound (heart murmur) through a stethoscope, or a large heart may be visible on an x- ray.
When a heart problem is suspected several tests may be used:
- pulse, blood pressure, temperature, and the number of breaths a child takes a minute
- listening with a stethoscope for changes in the heart sounds
- an oxygen saturation monitor to see how much oxygen is carried in the blood
- a chest x-ray may be taken to see the size and position of the heart
- an ECG (electrocardiogram) to check the electrical activity of the heart
- an ultrasound scan (echocardiogram) to see how the blood moves through the heart
- tests on blood or urine to assess the ‘chemical balance’ within the body
- a catheter or Magnetic Resonance Imaging scan (MRI)
- exercise testing – to check the breathing, blood pressure and rhythm during exercise on a treadmill (if possible).
Treatment
Treatment cannot cure DCM, but medicines can help your child’s heart to stabilise, and in many cases medicines reduce the risk of the condition getting worse. It is possible that your child may recover spontaneously.
- Drugs: ACE inhibitors, antiarrhythmics, beta-blockers, digoxin, diuretics and anticoagulant can all treat symptoms and improve the heart’s efficiency to pump blood around the body.
- Pacemaker – If your child’s heart rate is too slow, a pacemaker may be needed.
- Implantable Cardioverter Defibrillators (ICD) – in rare cases an ICD can be implanted to shock your child’s heart out of a dangerous fast rhythm.
Heart Transplant
If your child’s condition cannot be controlled using these treatments he or she may be assessed for a heart transplant.
For further support please contact the Cardiomyopathy UK at: 0800 018 1024 or visit their website: www.cardiomyopathy.org
Evidence and sources of information for this CHF information sheet can be obtained at:
(1) NHS Choices. Warfarin. London: NHS; 2017. Available at:
https://www.nhs.uk/medicines/warfarin/
(2) National Institute for Health & Care Excellence. Implantable Cardioverter Defibrillators and Cardiac Resynchronisation Therapy for arrhythmias and heart failure. London: NICE; 2017. Available at
www.nice.org.uk/guidance/ta314
(3) Cardiomyopathy UK: Information about Dilated Cardiomyopathy. London: Cardiomyopathy UK; 2017. Available at:
(4) NHS Choices. London: NHS; 2017. Available at
www.nhs.uk/conditions/cardiomyopathy/Pages/Introduction.aspx#dilated
About this document:
Published: Oct 2014
Reviewed: May 2022
To inform CHF of a comment or suggestion, please contact us via info@chfed.org.uk or Tel: 0300 561 0065.









