Atrioventricular Septal Defect (AVSD)
Download this information sheet as a PDF
The aim of this information sheet is to explain what Atrioventricular Septal Defect (AVSD) is, what effect it will have on a child and how it can be treated.
What is Atrioventricular Septal Defect?
- Atrioventricular means ‘of the atria and the ventricles’ – the four chambers of the heart.
- Septal means ‘of the septum’ – the wall between the left and right sides of the heart.
- Defect refers to a hole.
So Atrioventricular Septal Defect means there is a hole between the atria and between the ventricles.
In a normal heart there is a mitral valve between the left atrium and ventricle and a tricuspid valve between the right atrium and ventricle.
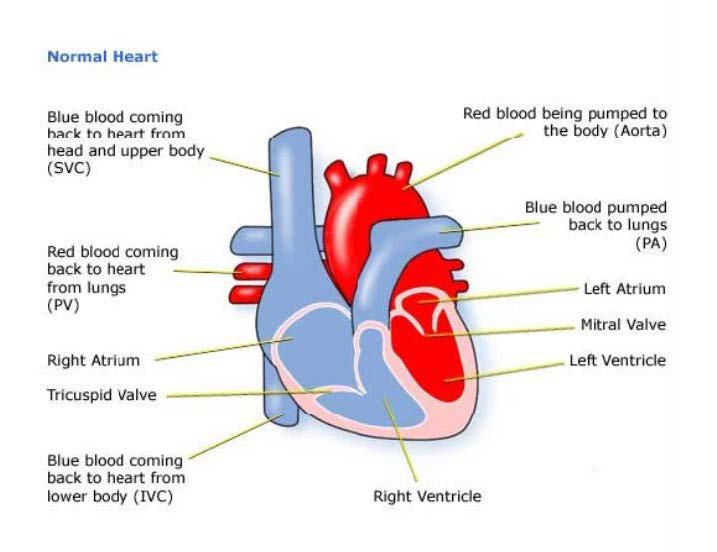
Hearts affected by AVSD only have one atrioventricular valve (see Figure 1).
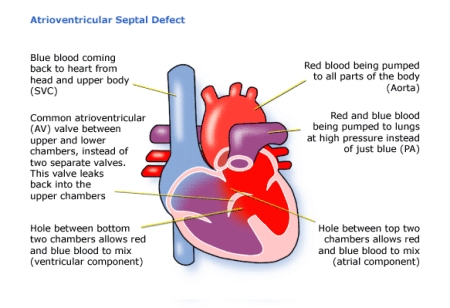
The blood on the left side of the heart is at higher pressure than the blood on the right side of the heart. This means that oxygenated blood flows from the left side of the heart, through the holes and mixes with the deoxygenated blood on the right side of the heart. The result is that there is too much blood on the right hand side of the heart. This blood then has to flow at high pressure into the pulmonary artery towards the lungs.
The one atrioventricular valve often leaks either into the left or right atrium or both. This makes the heart less efficient than normal so it has to work harder to function.
Figure 1 shows a complete AVSD. AVSDs can also be ‘partial’ or ‘intermediate’. In a partial AVSD there is only a hole between the atriums and there are two valves, although the mitral valve is deformed and often leaky. In an intermediate AVSD there is a small hole between the ventricles.
Diagnosis
AVSD can be diagnosed before birth during a pre-natal scan. AVSD’s are common in children with Down Syndrome. Therefore, if your child has Down’s Syndrome, his or her heart may have been examined to check for an AVSD. If your child’s heart condition is very complex the AVSD may be just one of a number of defects.
After they are born, babies with AVSD may have a bluish tint to their skin and they may be breathless and have problems feeding. Feeding problems can mean that the baby has difficulty putting on weight and babies with AVSD are also prone to chest infections.
Babies and children with AVSD will also have heart murmur. The murmur is the sound of the extra blood being pushed towards the lungs and leaking through the valve.
If your child has the partial or intermediate form of AVSD there may not be any symptoms early in life, other than a heart murmur.
When a heart murmur is heard the tests used can be:
- pulse, blood pressure, temperature, and number of breaths a baby takes a minute
- listening with a stethoscope for changes in the heart sounds
- an oxygen saturation monitor to see how much oxygen is getting into the blood
- a chest x-ray to see the size and position of the heart
- an ECG (electrocardiogram) to check the electrical activity
- an ultrasound scan (echocardiogram) to see how the blood moves through the heart
- checks for chemical balance in blood and urine
- a catheter or Magnetic Resonance Imaging test may be needed
Treatment
Once an AVSD is diagnosed the child will be carefully monitored to see when they need surgery. If the heart is not able to operate properly then parents may be told that their child is in ‘heart failure’.
Symptoms of heart failure include the lungs and other organs becoming heavy or ‘wet’ with fluid. A careful check will be kept on the child’s weight as any increase can be due to fluid retention. To help get rid of the extra fluid the child may need special medicines called diuretics.
A complete AVSD causes pulmonary hypertension (high pressure of blood in the lung arteries), and an operation will need to be performed before the lungs are damaged.
This operation is open heart surgery, which means that the heart will need to be stopped and opened to repair it. A heart bypass machine will take over the job that the heart normally does.
The aim of the operation is to make the circulation of blood through the heart and lungs normal. A patch is put over the holes between the atria and ventricles. The single atrioventricular valve is then divided to make two effective valves.
If a child has other heart defects, the kind of surgery needed will depend on how the heart can best be modified to cope with all the problems he or she has.
For most children this surgery is low risk, but it can depend on how well your child is otherwise. The doctors will discuss risks with you in detail before asking you to consent to the operation.
The length of time in hospital will usually be only 10 to 12 days, of which one or two will be spent in the intensive care and high dependency unit. Of course this depends on how well your child is before and after the surgery, and whether any complications arise.
If the surgery is straightforward, and your child does not have other health problems, he or she should be completely well shortly after surgery. There will be a scar down the middle of the chest, and there may be small scars where drain tubes were used. These fade very rapidly in most children, but they will not go altogether. Smaller scars on the hands and neck usually fade away to nothing.
How it affects your child
Some of these problems can occur after surgery or later in life:
- It is common for the valves to leak a little. If this becomes severe, they may need to be repaired or even replaced with artificial valves.
- If an artificial valve is inserted then the child will need to take an anticoagulant medicine to stop blood clots forming.
- The electrical system of the heart is sometimes damaged during surgery. This can cause a slow heartbeat, called heart block. This may need to be corrected by giving the child a pacemaker.
- Some patients go on to develop sub-aortic stenosis, a blockage below the aortic valve, which may need to be repaired using open heart surgery.
Evidence and sources of information for this CHF information sheet can be obtained at:
(1) Downs Heart Group
Atrioventricular Septal Defect with Fallot’s Tetralogy. London: Downs Heart Group; 2017. Available at:
http://www.dhg.org.uk/information/avsdfallots.aspx
(2) European Heart Journal
Familial co-occurrence of congenital heart defects follows distinct patterns
Sabrina G. Ellesøe, et al. 2017. Available at:
https://doi.org/10.1093/eurheartj/ehx314
About this document:
Published: June 2013
Reviewed: May 2022
To inform CHF of a comment or suggestion, please contact us via info@chfed.org.uk or Tel: 0300 561 0065.









