Sam's Story
told by mum
Samuel was born at full term after an uneventful pregnancy. We had had a quick discharge from hospital, so our GP visited us at home the following day and a full newborn examination did not reveal anything unusual. Samuel was very quiet, rarely cried and slept beautifully. My only complaint with him was his feeding. Although I was bottle feeding it was difficult to get more than an ounce of milk into him at a time. We would have to dedicate an hour to feeding him and it often became a battle to keep him awake or get any milk into him at all.
When he was two weeks old, I took him to see our health visitor who quickly dismissed my concerns. Without looking at Samuel she simply said that she sensed some anxiety and I ‘needed to learn not to put my mental health problems onto my baby’. I was devastated by this reaction and wondered if it was all my fault.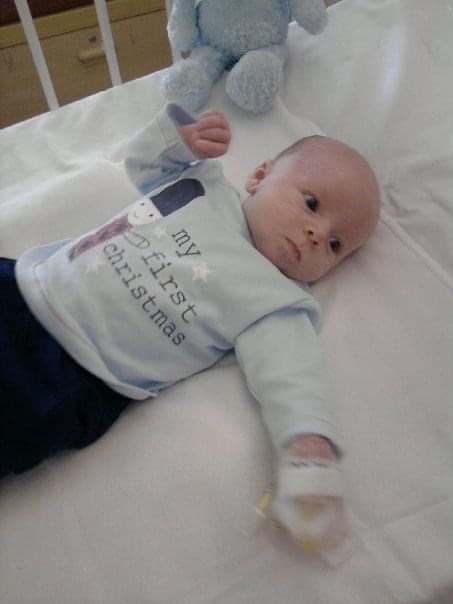
Over the next two weeks I saw the health visitor twice more and again was told there was nothing wrong with him. The last occasion was at baby clinic. I’d gone armed with a list of how much milk Samuel had had over the previous few days. I knew it wasn’t enough. I showed her the list, Samuel was weighed, and he had put on weight. I was then told if my list was correct then ‘he wouldn’t be putting on weight, would he?’ Again, I was left upset at the realisation that they simply did not believe me. His breathing appeared fast at this appointment, and they felt that he had a cold and advised me to see our GP.
We went to the doctors that evening and soon found ourselves on the way to our local hospital. Here they felt he had bronchiolitis and decided to keep him in overnight for observation. We were asked many questions about his feeding. The doctors believed me about the poor quantities but asked repeatedly why I had failed to do anything about it. This added to my upset as I’d spent two weeks raising concerns without anyone taking me seriously and now felt I was being seen as neglectful. Overnight Samuels oxygen saturations deteriorated, and he was put onto oxygen.
The ward round the next morning brought a new team of doctors and one thought he heard a slight heart murmur. We were reassured that this was probably nothing. An echo would be arranged, and we shouldn’t worry about it. Later that day Samuel went for the echo and the rest is history.
It was found that he had critical aortic stenosis, was in severe heart failure and was actually very seriously ill and soon afterwards he had a cardiac arrest. He needed to be ventilated but his heart failure was too bad. He was put onto CPAP and we were told that we simply had to hope for the best. They struggled to find an intensive care bed for him. The closest one was in central London 70 miles away. We had had heavy snow that day and during the evening severe fog had set in. A helicopter transfer was not a possibility and London was deemed too far – Samuel was unlikely to survive the journey. Eventually a bed was found at Oxford which was closer. He was transferred there but again we were warned that there was a possibility that he would die on route.
He made it there safely though with no drama. The following day he had a balloon valvoplasty and returned from theatre as completely different baby. He cried, he was awake, he smiled, he made noise and he would down a complete bottle of milk in about 15 minutes. He was discharged home on Christmas Day.
I had a huge amount of anger over his delayed diagnosis. I had felt dismissed and made to feel at fault over his condition. As a nurse I was horrified at myself that I failed to notice my own child was in severe heart failure. I also know that had he arrested at home his chances of survival would have been almost non-existent.
Despite being the most common birth defect there was such little awareness. I knew nothing of CHD myself. My health visitor had told me in detail all about the very rare disease that the heel prick test looks for but was completely unaware that he was showing the classic symptoms of a heart defect.
As he grew, his valve deteriorated, and he then had severe aortic regurgitation. When he was 7 he had open heart surgery for an Ozaki procedure where they created a new valve for him using his own pericardium. The hope was that this would last for 10 years but sadly the leaflets of the valve fused a few months after surgery. He managed symptom free for nearly 5 years when he began to deteriorate again.
Samuel began to get chest pain and quickly became very limited in the activity he could do. Apart from going to school, he wasn’t allowed to go much else! We were told that Samuel again had severe aortic stenosis and it was decided that his valve needed urgent attention.
The week before his 13th birthday he had surgery to have a mechanical aortic valve inserted along with a reconstruction of his aorta which had become dilated as a result of the stenosis. He had a very quick recovery, but he was in hospital for a little while as he now needed to take warfarin and we needed to get to grips with testing as well as ensuring his warfarin levels were correct.
He came home after nearly 2 weeks in hospital. We were given an INR machine so that Samuel can test his own blood at home and then we speak to the hospital to get the warfarin dose. He tests roughly twice a week and the machine at home means it is more convenient to test- no visits to the hospital. We can also quickly test if we have any worries as his INR can be affected by many things – colds, foods, excessive activity…..

Since he had been on warfarin, he’s managed a residential trip away with school and whilst we have to careful with a few things, warfarin hasn’t limited what he does, and we’ve adjusted to it well. Physically he is back to normal with no limitations or pain, and we are keeping our fingers crossed that this valve lasts a long time for him.
If you have been affected by any of the issues raised in this content you can contact info@chfed.org.uk or 0300 561 0065.









